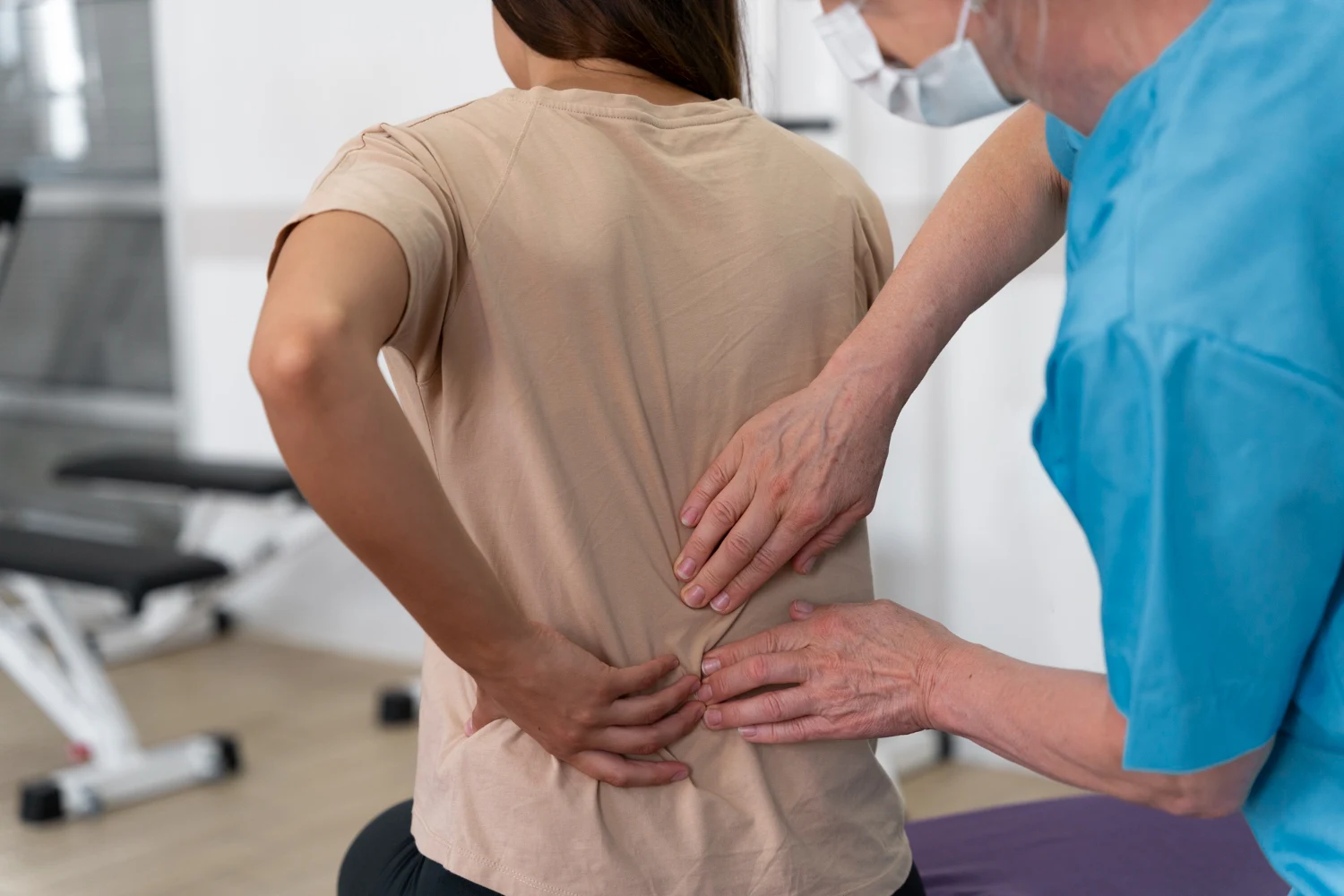
Lower back pain is one of the most common health problems affecting people of all ages. It can interfere with daily activities such as walking, sitting, working, or even sleeping. In many cases, lower back pain develops gradually due to poor posture, muscle strain, or lifestyle habits.
Understanding the common causes of lower back pain is the first step toward effective treatment. Physiotherapy is one of the most recommended and effective treatments because it helps reduce pain, strengthen muscles, and restore proper movement without the need for surgery or long-term medication.
What is Lower Back Pain?
Lower back pain refers to discomfort or pain in the lumbar region of the spine, which is the lower portion of the back. This area supports most of the body’s weight and plays an important role in movement and stability.
Lower back pain can range from mild discomfort to severe pain and may be short-term (acute) or long-term (chronic).
10 Common Causes of Lower Back Pain
1. Poor Posture
Sitting or standing with incorrect posture puts excessive pressure on the spine and surrounding muscles. Over time, this strain can lead to chronic lower back pain.
- Slouching while sitting.
- Working long hours at a desk.
- Improper sleeping positions.
2. Muscle Strain
Overstretching or tearing of back muscles due to heavy lifting or sudden movements can cause muscle strain, leading to pain and stiffness in the lower back.
- Lifting heavy objects incorrectly.
- Sudden twisting movements.
- Overexertion during exercise.
3. Herniated Disc
A herniated or slipped disc occurs when the soft inner portion of a spinal disc pushes through its outer layer. This can press on nearby nerves and cause severe lower back pain.
- Pain radiating to legs.
- Numbness or tingling.
- Weakness in muscles.
4. Sedentary Lifestyle
Spending long hours sitting with little physical activity weakens the core and back muscles, making the spine more vulnerable to injury and pain.
- Long hours of desk work.
- Lack of regular exercise.
- Poor muscle strength.
5. Obesity
Excess body weight puts additional pressure on the spine and lower back muscles, increasing the risk of back pain.
- Higher stress on spinal joints.
- Reduced mobility.
- Increased risk of chronic pain.
6. Degenerative Disc Disease
As people age, spinal discs gradually lose flexibility and cushioning ability. This condition can lead to chronic lower back pain and reduced mobility.
- Age-related disc wear.
- Reduced spinal flexibility.
- Persistent back discomfort.
7. Sciatica
Sciatica occurs when the sciatic nerve becomes compressed or irritated, usually due to a herniated disc or spinal problem. It causes pain that radiates from the lower back down the leg.
- Sharp shooting pain.
- Numbness in legs.
- Burning sensation along the nerve.
8. Injuries or Accidents
Sports injuries, falls, or car accidents can damage muscles, ligaments, or spinal structures, leading to lower back pain.
- Sudden trauma to the back.
- Ligament injuries.
- Spinal misalignment.
9. Stress and Muscle Tension
Emotional stress can cause muscles in the back to tighten, which may lead to persistent pain and stiffness.
- Muscle tightness.
- Poor body posture during stress.
- Reduced relaxation of muscles.
10. Weak Core Muscles
The core muscles support the spine and maintain proper posture. Weak core muscles can lead to instability and increased strain on the lower back.
- Poor spinal support.
- Higher risk of injury.
- Reduced balance and stability.
How Physiotherapy Helps Treat Lower Back Pain
Physiotherapy is a safe and effective treatment for lower back pain. It focuses on improving mobility, strengthening muscles, and correcting posture to reduce pain and prevent future injuries.
Benefits of Physiotherapy
- Reduces pain and inflammation.
- Strengthens back and core muscles.
- Improves flexibility and mobility.
- Corrects posture and movement patterns.
- Prevents recurring back pain.
Common Physiotherapy Treatments for Back Pain
Exercise Therapy
- Strengthening exercises for core and back muscles.
- Stretching exercises to improve flexibility.
- Movement training for better posture.
Manual Therapy
- Hands-on techniques to improve joint movement.
- Muscle relaxation techniques.
- Spinal mobilization.
Posture Correction
- Training to maintain correct sitting and standing posture.
- Workplace ergonomic advice.
- Education on safe lifting techniques.
Pain Relief Techniques
- Heat or cold therapy.
- Ultrasound therapy.
- Electrical stimulation therapy.
Conclusion
Lower back pain is a common condition that can affect people of all ages. It often develops due to lifestyle habits, muscle weakness, injuries, or spinal problems. Identifying the cause of back pain is essential for effective treatment.
Physiotherapy plays an important role in managing and preventing lower back pain. Through targeted exercises, posture correction, and pain relief techniques, physiotherapy helps restore mobility, strengthen muscles, and improve overall spinal health.
With proper care and regular physiotherapy, most people can significantly reduce lower back pain and return to a healthy, active lifestyle.